Why I Added Detailed Advanced Directives to my Living Will

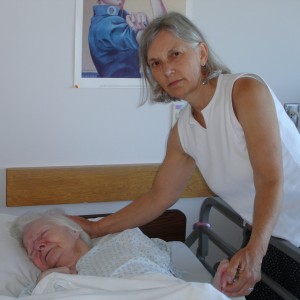
“What’s wrong?” I asked Patty. Patty was Mom’s aide at the skilled nursing home. She wore colorful smocks with floral prints and always smiled, but not today. Aides stood around in quiet clumps with frowns on their faces. Had someone died?
“There’s a patient we can’t feed. Everyone’s upset,” Patty said.
“Why can’t you feed her?” I asked. My heart pounded as I waited for her answer. My mom had been lying in a fetal position for years, unresponsive and comatose. All that was left of her was bones and a swallow reflex. They put a straw to her lips and she sucked. They put gruel in her mouth and she swallowed.
“The woman had a stroke and her Advanced Directives says we can’t feed her or give her water if she doesn’t respond,” Penny said with a sad shake of her head.
“But Penny, that’s what should happen to my mom.”

“Maybe. But we’re trained to feed people. It’s upsetting to let a patient die.”
“Is her life worth living?”
“The woman already decided no. That’s hard for us,” Penny said.
My mother had a Living Will and a Do Not Resuscitate order, but nothing to guide the nursing home in this situation. Mom, both her siblings, and my grandmother had Alzheimer’s Disease by their late 70s. I fretted about being stuck in limbo for many years like my mother and grandmother.
“A patient wrote in her living will that she can’t be fed if she is unresponsive and doesn’t indicate that she wants food,” I told my husband Vic when I got home. “She had a severe stroke and hasn’t responded for a month. Her kids support her directives. It’s legally binding, so the nursing home has to comply.”
“I didn’t know you could do that,” Vic said.

“Me either, but I’m doing it. Are you in?”
“Definitely,” he said. I made an appointment with our doctor, the medical director of the nursing home.
“Would I suffer more without water or food?” I asked.
“No, both are gentle ways to die.”
“Can we do this legally?” I asked.
“Yes,” our doctor said. “I’ll help you word it.
We amended our living wills with these words: “If I have dementia, severe neurological illness, permanent severe mental disability, permanent unconsciousness, or end stage terminal illness, I want comfort care only.”

Under optional additional directives, we added: “If I have irreversible mental damage from dementia or other brain damage and cannot feed myself and do not ask for food or water for one month, I wish to die. Do not feed me food or water by mouth, tube, or intravenously so that I can die naturally and quickly. I ask that this directive be enforced by my health care agent and carried out by those who care for my body.”
Our doctor suggested the one month delay for the sake of those making final decisions. This would give everyone adjustment and monitoring time if needed, but not too much. Rather than an ICU death, I chose an untethered quiet death.
We wrote our directives by hand, signed, and went home with a great sense of relief. I couldn’t help my mother leave her spent body and mind, but hoped to save myself from my mother’s fate.
***
See Caring Connections page to download living will and advanced directive guides and forms for your state. For more articles about my mother and me, see From Medicine to Mercy or My Mother’s Blessing.



October 9, 2020 at 11:54 am
Chris Pederson
I am scared about being stuck in a limbo-like situation with Alzheimer’s as well. My family has a long history with it and I’ve been told it can be hereditary. I like your advice to get a living will that allows for you to be taken care of but not kept alive for a long time once you get the disease.
October 10, 2020 at 11:50 am
Elaine Mansfield
I’m glad my article helped, Chris. It’s an alarming possibility for all of us. It’s also essential to have those hard conversations with those who will be in charge when we can’t decide. My mother didn’t do that and her second husband overrode her DNR. Her last years were deep misery for her. I don’t want that to happen to me if I have severe dementia and can’t decide for myself, so my two sons know what I want and I remind them every year. There may be a time when I can’t remind them, but I trust them to remember.
July 24, 2017 at 4:24 am
susan scott
Thanks Elaine – an important post and a reminder that we need to address death, not only our own but those of family, and friends too if they have no family to attend to their end-of-life wishes. Here in South Africa we have ‘A Living Will’ which my late father-in-law had. My husband and I have discussed it but I don’t think we’ve put it down on paper and had it legalised.
Yes, it’s true that the medical profession’s task is to uphold/preserve life, the Hippocratic Oath. Are they caught in a bind? I suspect so …
I loved the comments too and your response back to them.
July 24, 2017 at 10:29 am
Elaine Mansfield
Thank you, Susan. Watching my own mother wither for 10 years was a huge motivation for Vic and me to put things in writing. Our internist and good friend was also the medical director of my mother’s nursing home, so he helped us with wording.
I know that directives aren’t always followed even when they’re clear, but we can make it more likely that they are if we write things down, choose a health care proxy, and talk to them. After my request (not at the doctor’s suggestion, but he agreed to my observations), my mother-in-law was referred to Palliative Care with Hospice about three months ago. Recently, again at the request of me and her health aides and after innumerable mishaps, her doctor put in an order for hospice care. The health aides and I are relieved. My mother-in-law’s care won’t change much, but it might improve because we’ll have expert support from people who know how to read what’s going on and help us make her more comfortable. We are all in a bind about how to die with medicine offering so many ways to hold off death for just a little longer.
August 2, 2014 at 8:31 am
Haywood Rhodes
This is an excellent point Elaine. I am in healthcare and see so much prolonged suffering and added expense to our healthcare system because families have not appropriately addressed end-of-life care. I think part if this is due to the American culture and the sense we can overcome anything, but a lot of it is just ignorance about what end-of-life care and dying with dignity entails. Thanks so much for helping to educate others about this process.
August 2, 2014 at 8:55 am
Elaine Mansfield
Haywood, thank you for your thoughts. I agree we think we can overcome anything and we are afraid to mention the possibility of death, even when someone is obviously dying. Somehow death, as inevitable as it is, has become a failure. When it’s difficult to get people to accept the idea of mortality, it’s impossible to educate them about end-of-life care. My husband had cancer and a realistic view of his chances, but cancer often involves warrior oncologists who have one more experimental drug to try. It was tricky choosing the right moment to say enough, but without a realistic look at his situation and an acceptance of mortality, he would have spent a long time on life support. That didn’t happen.
As you probably know, there’s a growing interest in learning more about mortality and educating oneself about death. Since it’s driven by young people (Death Cafe movement, for example), it may take hold. Thanks again.
July 30, 2014 at 2:37 pm
Shirley Hershey Showalter
Elaine, I found this post both inspiring and a bit of a kick in the pants. I need to print out the language you so helpfully provided and discuss with our doctor. Fortunately, my annual check up comes soon.
My mission, to prepare for the hour of my death one good day at a time and to help others do the same, is totally relevant.
Love the photos and layout of your blog space.
July 30, 2014 at 3:02 pm
Elaine Mansfield
Shirley, a kick in the bottom isn’t a bad thing in this context. I think doctors are the best resources for what’s most binding in your state. I made an appointment completely dedicated to advanced directives since there is never enough time in a doctor’s visit.
Our years of spiritual practice and Vic’s last two years devoted to the Dalai Lama’s practice of kindness prepared us both for his death and me for mine. It was still heart-breaking, but I felt powerful support almost all the time. I’ll keep on practicing.
Thanks for noticing my blog layout and photos. It’s a way to create and share beauty. I like finding images almost as much as I like writing the pieces.
July 26, 2014 at 11:26 pm
Ann Napoletan
Thank you for sharing your story, Elaine. Like you, I have my wishes written into my advance directives, and I wouldn’t have it any other way. I’m beyond grateful to my mother for having the foresight to to this as well – long before dementia was even a blip on our radar. I believe it’s one of the greatest gifts we can give our loved ones.
As you know, my mom’s final 9 days were spent in a wonderful hospice facility. Having gone through that experience, I know how difficult it was to literally watch her melt away and how – at times – it felt so wrong not to give her fluids via IV. I had to continually remind myself that we were following HER wishes.
Although I knew all quality of life was gone, human nature is that we want to fix things. It feels wrong to do nothing. But there comes a time when doing nothing is exactly the right thing to do. I’ll never forget the evening one of her caregivers who had become like family to us looked at me and said, “You can go against her wishes, you know.”
I couldn’t believe what I was hearing, but for a split second I began to have doubts. Maybe I should ask for artificial hydration and nutrition. Thankfully, it was only a brief moment, and then I reminded myself that would be selfish. My mom was at the end of her rope; worn out and exhausted. To keep her alive at that point would have been cruel and self-serving. She was ready even if I wasn’t…
Much love to you, Elaine. I plan to write a brief post on my blog and include a link to this piece. I don’t think we can remind people too often – for the sake of your loved ones, get your advance directives in order. Don’t leave them with those agonizing end of life decisions. Make your wishes known.
July 27, 2014 at 8:19 am
Elaine Mansfield
Ann, what a wonderful gift you gave your mom by standing by her directives–and showing everyone how easy it is to decide not to follow them. We have to make sure our health proxy is behind us 100%, and if our health proxy doesn’t think they can stand by our decisions in a pinch, important to give someone else that role.
Thank you for posting a link to my article at your site. Alzheimer’s Disease is a medical issue that lends itself to the need for Advanced Directives. It’s easiest to assume we won’t have dementia, but if we wait to find out then it could be too late. I don’t make assumptions either way, but I’m prepared. I think on my local Hospicare motto: “It’s about how you live.”
July 25, 2014 at 3:29 pm
Deb Kosmer
Thank you Elaine for sharing this vital and needed information. Having clear precise advanced directives is one of the best gifts we can give to ourselves and our loved ones. It eliminates ambiguity even if some loved ones don’t agree with it. Working in hospice for 12 years and several with older adults, along with personal experiences with family members have solidified my feelings about end of life decision making. Deb Kosmer
July 25, 2014 at 4:28 pm
Elaine Mansfield
Yes. It’s so important to reinforce this because everyone naturally says, “Later.” You, more than I, know that later may never come. Thank you for the wonderful work and writing you do.
July 24, 2014 at 11:49 pm
Debby Gies
Great information Elaine and told with such compassion. My husband and I made wills over a decade ago and we included directions for a living will then. I’d also mention that it is a good idea to revisit our will every so many years because situations change and we may need to update our wishes. 🙂
July 25, 2014 at 9:09 am
Elaine Mansfield
I agree about revisiting our living wills, Debby. And I plan to do that. My wishes haven’t changed, but the first comment alerted me to something new in New York State that may be more legally binding than advanced directives. I’ll ask my doctor and see what he says. Thanks for your comment and support.
July 26, 2014 at 7:38 pm
Debby Gies
You are welcome. Thanks for sharing the important post which many would rather not think about. 🙂
July 24, 2014 at 10:24 pm
Greet Grief
Oh what sweet pictures of you and your mom! And what great information to share and such an important conversation to be had. We all need to have the empathy for our loved ones to do the work for them before they are placed in a position to have to make these difficult decisions. It is the final gift we can give our loved ones – decisive, clear directions from our heart to theirs. I will be reviewing my instructions because of this post – thank you!
July 25, 2014 at 9:07 am
Elaine Mansfield
My husband took many photo of my mom and me. He was an excellent photographer with a good eye.
Yes, decisive and clear directives are a gift to those we love and a gift to ourselves. We may never need them, but in certain situations, they’re invaluable. We didn’t use them with my husband because until the last few days he could make decisions for himself. Then I decided based on what I knew he wanted when his illness could no longer be treated. In light of some of the feedback in comments, I’m revisiting this issue with my doctor, too. It’s been ten years since I made these directives and there may be better options now. Thank you, Kathy.
July 23, 2014 at 7:25 pm
Gilly
Thank you for writing about this important and difficult topic Elaine. I think you will help so many people by sharing your exact wording. That is hard to work out and compose.
When I volunteered and then worked at hospice, I saw first hand how advanced directives helped people to retain some control at the end of their lives and lifted the burden of decision making off their loved ones. In fact it was a gift to them, because they knew what the person who was dying wanted and they could honor it. I have tried to have these conversations with my mom. She is not interested in making this kind of commitment now. I just hope she will let my sister and I know, what she wishes for most for the end of her life, while she is still healthy. Gilly
July 23, 2014 at 10:17 pm
Elaine Mansfield
You’re so right, Gilly. I see this as a gift to my children as much as anything else. I was caught in the not dead but not really alive limbo with my mother for too many years, and I know she did not want to end up in that place.
My mother-in-law is 98. She is amazingly together mentally. Physically, she’s strong, although she’s blind. She’s always been unwilling to have “the conversation.” She does has a DNR and I’m her health care proxy, so it looks like I’ll be the one making the decisions.
Thanks for telling me a little more about you in the process of making a comment.
With appreciation, Elaine
July 23, 2014 at 11:25 am
Mary Friedel-Hunt
Elaine, this is such an important piece. I am going to get my papers out and make sure this is covered in them and if not, they will be updated. Thank you for this. I know you will help many with this piece.
July 23, 2014 at 12:30 pm
Elaine Mansfield
Thanks, Mary. If you read other comments here, you’ll know there might be new options and resources, depending on where you live. My living will was written 10 years ago, so I will revisit these options with my doctor. I think we’re better at creating advanced directives for our dogs than we are for ourselves.
July 23, 2014 at 9:57 am
Lynne Taetzsch
Thanks, Elaine, for making this so clear. Fortunately, Adrian had a living will that said clearly he did not want food or liquids (hydration) administered. We both put that in our living wills. It saved him from suffering in the end.
But with your updated information and others’ comments, I will recheck all this for myself.
July 23, 2014 at 10:22 am
Elaine Mansfield
Lynne, I’m glad to hear about Adrian’s directives and that they saved him from extra suffering. Since it’s been ten years since my advanced directives were written, I’ll also talk to my doctor about this again to make sure I have everything covered. Since my sons live out of state, I need a document that works nationally. A little more investigation is in order.
July 23, 2014 at 2:37 am
Dennis A. Dore
Thanks for this Elaine. I now know how to proceed on this end should those circumstances apply. Touching and helpful as always!
July 23, 2014 at 8:38 am
Elaine Mansfield
Dennis, circumstances apply because we are all mortal. And we’ve learned a lot from watching others die. Vic’s cancer death was not a lingering death and treatment only ended at the very end of his life. He was able to choose what he wanted until the last few days. My directives are most pertinent in a prolonged lingering death. If I can decide, good. If I can’t, I have a back-up plan. Look at Myra’s comment on this thread for more information.
July 23, 2014 at 1:47 am
Patti Hall
All we can do is spread the information, but your real life experiences add a sense of urgency that should help others (at least) start considering their options.
In my mid 50’s, I can’t think of many in my generation who haven’t had end-of-life decisions to make or witness, for themselves or loved ones.
Thanks again, Elaine!
P
July 23, 2014 at 8:33 am
Elaine Mansfield
Patti, you’re right on. Many of us have already had to make these decisions. We make it easy for those we love if we’ve figured out what we want and have it in writing. There are great ideas in this thread, some of them I didn’t know about. Thanks for your note and take care of yourself.
July 22, 2014 at 11:17 pm
Janet Wylde
Thank you Elaine. This is a good reminder. It’s so easy to put this kind of thing off yet so important.
July 23, 2014 at 8:31 am
Elaine Mansfield
I love hearing from you, Janet. We need to know what we want and what our parents want. I’m the health proxy for my mother-in-law and just yesterday the social worker where she lives wanted to confirm this. It seems the most important thing is to make sure your children know what you want and will stand by your decision.
July 22, 2014 at 10:46 pm
Myra Berkowitz
Dear Elaine & all,
It’s my understanding (somewhat limited) that POLST and MOLST are more binding than living wills, in states that have these in place. For more information, see:
http://www.polst.org/
For NYS, see:
https://www.health.ny.gov/professionals/patients/patient_rights/molst/
Love,
Myra
July 23, 2014 at 8:29 am
Elaine Mansfield
Myra, thank you for the important information. My directives may be a bit out of date since they were written ten years ago, but I have an appointment with my doctor in a few months and will ask about POLST and MOLST. Thanks for the links. Seems the most important thing is to face that we are mortal and figure out what we want to do about that. If we talk to our doctors or Offices of the Aging or a lawyer, we can figure out the best thing to do in our state. Thanks for guiding me and everyone in the right direction.
July 22, 2014 at 10:43 pm
Marty Tousley (@GriefHealing)
An important and timely piece, Elaine. Your readers might appreciate this article also: “Why It’s OK for Your Loved One to Stop Eating and Drinking on Hospice,” http://j.mp/1nSLzG5 ♥
July 23, 2014 at 8:25 am
Elaine Mansfield
Thank you, Marty, for the terrific and pertinent article. As a culture, we’re beginning to talk about what happens at death, and as we do, we’re moving toward allowing people to choose a less medicalized death. I’m grateful for so many signs of this.
July 22, 2014 at 8:55 pm
Robin Botie
This is so amazing, Elaine. And informative. Thank you for this. It must have been hard to write.
July 22, 2014 at 10:28 pm
Elaine Mansfield
Thanks, Robin. I’d written about my mom’s long lost years in a few places, so it was revisiting familiar ground. It’s sad what happened to my mom. I imagine she would have added the same things to her living will because she knew she had a risk, but no one gave her the option.
July 22, 2014 at 8:47 pm
Marian Beaman
What a timely post from first-hand experience with information so important to know. You will be saving those who read this from unnecessary sorrow for themselves and their loved ones. Cliff and I have an advance directive and so do my Mother and Aunt Ruthie.
Your most poignant phrase: an untethered quiet death . . . .
July 22, 2014 at 10:23 pm
Elaine Mansfield
Someone with Alzheimer’s in their family said on FB that she didn’t have a living will. I told her about mine. I thought others might want to consider additional directives. We have choices that no one discusses, but we have to make them while we can. The medical impulse is to save the body when all we have left is suffering. I understand that perspective, but it’s not what I want.
July 23, 2014 at 8:44 am
Peggy Keating
So important to know. Thanks Elaine!
July 23, 2014 at 10:19 am
Elaine Mansfield
Thank you, Peggy. And please read down the comments to see Myra’s addition to this. Most essential thing is to discuss what we want, let people know, and figure out how to get that in a legally binding form.